10 results
Moria or Mania? Manic symptoms as the clinical manifestation of glioblastoma recurrence: a case report
- F. Mayor Sanabria, M. E. Expósito Durán, M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. Paz Otero, I. Alberdi Páramo, B. Rodado León
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S520
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Up to 50% of patients with brain tumors experience psychiatric symptoms, and rates up to 80% have been reported in malignant neoplasms such as glioblastoma multiforme (GBM). Still, clinical presentation as mania-like syndromes is a rare phenomenon, mainly occurring when frontal structures are compromised.
We present the case of a 42-year-old woman who was admitted to our hospital due to manic symptoms coinciding with a recurrence of a bifrontal GBM, for which she underwent surgery 5 months prior.
Objectives1) To describe the clinical particularities of this case, focusing on the differential diagnosis.
2) To review the association between manic symptoms and frontal dysfunction caused by brain tumors, with special interest on GBM.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, we reviewed the available literature in relation to manic symptoms related to brain tumors.
ResultsThe patient’s GBM recurrence presented with late onset symptoms of mania, including euphoric mood, increased spending, ideas of grandiosity and hyper-religiosity. She had no previous psychiatric history but, interestingly, she had an extensive affective burden in her family, with 4 consummated suicides. However, she also presented other clinical signs, such as disorientation, perseveration, mild memory impairment and stereotyped motor behaviors, that pointed to relevant frontal lobe dysfunction, suggesting Moria as a possible contribution for the symptoms described.
Manic symptoms in the context of brain tumors appear in 7-15% of patients with psychiatric symptoms, usually associated with right frontal dysfunction (75% of cases). Bifrontal affectation, such as this patient, is only described in 6% of cases. Although fast growing, malignant tumors have been associated with higher rates of psychiatric symptoms, no correlation has been described between these and brain tumor histology.
Conclusions- The presence of atypical manic symptoms, such as those presented in this case, should raise clinical concern for secondary mania.
- Moria shares similarities with mania, including mood elevation, tendency to hilarity or hyper-sexuality, that may hinder diagnosis of patients with frontal dysfunction.
- This case outlines the difficulties in making a differential diagnosis in patient with both manic and neurological signs, and highlights the implication of frontal structures in the development of manic symptoms.
Disclosure of InterestNone Declared
Cultural factors in depressive experience and its severity: A case report
- C. Regueiro Martín-Albo, F. Mayor Sanabria, E. Expósito Durán, M. Fernández Fariña, M. Navas Tejedor
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S816
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For a very long time, anthropologists and psychiatrists have studied how the symptomatology of mental diseases varies among cultures. Different social environments approach depression in different ways, and cultural practices and meanings influence how it develops. Culture also affects how symptoms are felt and described, how treatments are chosen, how patients and doctors interact, how likely it is that certain events, like suicide, will occur, and how professionals behave. As a result, all of these circumstances must be taken into consideration when approaching the diagnosis and management of depressive disorders. To illustrate the above, we present the case of a 31-year-old man, originally from Nigeria, who was admitted to the hospital after a suicide attempt by precipitation onto the subway tracks.
Objectives(1) To describe the clinical particularities of this case, focusing on the diagnostic difficulties we faced derived from intercultural contrasts (2) To review cross-cultural differences in the symptomatology and its implication on severity of depressive disorders.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, a bibliographic review of the available scientific literature was also performed in relation to transcultural depressive experiences and its severity.
ResultsThere is little evidence in favor of a direct link between sociocultural factors and severe depression, but we reviewed the arguments that look significant for further research. Depressive illnesses are found in all societies and their symptomatic expression varies culturally, particularly in terms of somatization and delusional ideas. Similarly, the social and individual representations of the disease depend on the culture, and some conceptual models can increase the effects of stigmatization. These cross-cultural variations could influence the care-seeking process and therefore modulate the evolution of the disease in the sense of greater severity.
ConclusionsAll societies experience depressive disorders, which exhibit symptoms that vary culturally, especially in terms of somatization and delusional beliefs.
The care-seeking process is affected by cross-cultural differences, and as a result, the disease’s progression may also be modulated in terms of increased severity.
When we ignore cultural factors in understanding, assessing, and treating depression, we are contributing to misdiagnosis and errors in patient management.
Disclosure of InterestNone Declared
Visual hallucinosis and Linezolid use: A case report.
- M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. E. Expósito Durán, F. Mayor Sanabria, Í. Alberdi Páramo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1012
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 78-year-old man with multiple somatic pathologies and associated depressive symptoms, under treatment with Citalopram 10mg, who was admitted due to cholangitis secondary to biliary prosthetic obstruction.
Empirical antibiotic treatment with Meropenem and Linezolid was started, along with an increase in the dose of Citalopram to 20mg due to mood worsening. The patient begins with symptoms consisting of complex and polymorphic visual hallucinosis, without any affective or behavioral repercussions. He does not present another semiology of the psychotic sphere.
ObjectivesTo highlight the importance of knowing the different interactions and adverse effects of drugs for good clinical management.
MethodsWe collected the complete medical history of our patient and we carried out a review of the interactions and adverse effects described with the antibiotic drug Linezolid.
ResultsAs the onset of hallucinations was temporarily correlated with the use of medications, drug-induced hallucinations were suspected, resolving completely after 2 days after withdrawal of Linezolid treatment.
Linezolid is a nonselective inhibitor of MAO A and B, preventing the destruction of monoamine neurotransmitters like serotonin, dopamine, or norepinephrine. It has dopaminergic properties that may enhance the central nervous system effects of anticholinergics and co-prescription with serotonergic drugs increases the risk of serotonin syndrome.
ConclusionsThis case highlights the importance of taking into account drug interactions and adverse effects to reduce the risk of drug induced symptoms and optimize their management.
The increase in resistance to antibiotic treatment allows us to anticipate that the use of Linezolid will increase in the coming years, and it is important to know its mechanism of action given the interactions with psychotropic drugs that we use in our usual clinical practice
Disclosure of InterestNone Declared
Cyclothymia, bipolar disorder and multiple sclerosis: A case report
- M. D. P. Paz Otero, E. Lozano Bori, J. Sánchez Rodríguez, S. Puyal González, M. Fernández Fariña, F. Mayor Sanabria, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S703-S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 49-year-old woman who was diagnosed with multiple sclerosis at the age of 19 and suffers from an affective disorder that has been evolving for years. This condition, for which she has been followed by psychiatry and psychology for more than ten years, consists of alternating periods of hypomania lasting weeks and phases in which frank depressive symptomatology predominates, with no phases of euthymia in between and with a predominance of severe deterioration of her functionality at both poles.
Objectives(1) We will review the term cyclothymia and explore the concept of “cyclothymic temperament” advocated by some authors, in order to be able to understand the dimension of the present case and reformulate its approach.
(2) The relationship between multiple sclerosis and bipolar spectrum disorders will be covered, reviewing the current knowledge in this regard and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, taking into account her life history, the complementary tests performed as well as the multiple therapeutic approaches tried over the last few years.
Likewise, a bibliographic review of the available scientific literature will be carried out in relation to the diagnosis of cyclothymia or bipolar disorder type II, the controversial term “cyclothymic temperament”, and the relationship that these diagnoses have with the diagnosis of Multiple Sclerosis.
Results(1) Our patient could fit into what many authors define as a cyclothymic temperament, fulfilling, in certain episodes, the criteria that the manuals propose for bipolar disorder type II.
(2) 2.1 The prevalence of bipolar affective disorder in MS is approximately twice as high as in the general population (rates of 0.3-2.4%). 2.2 Patients with MS have higher scores in cyclothymic and hyperthymic temperament than the control group. 2.3 Certain drugs generally used in BD also seem to have a beneficial effect on MS.
Image:
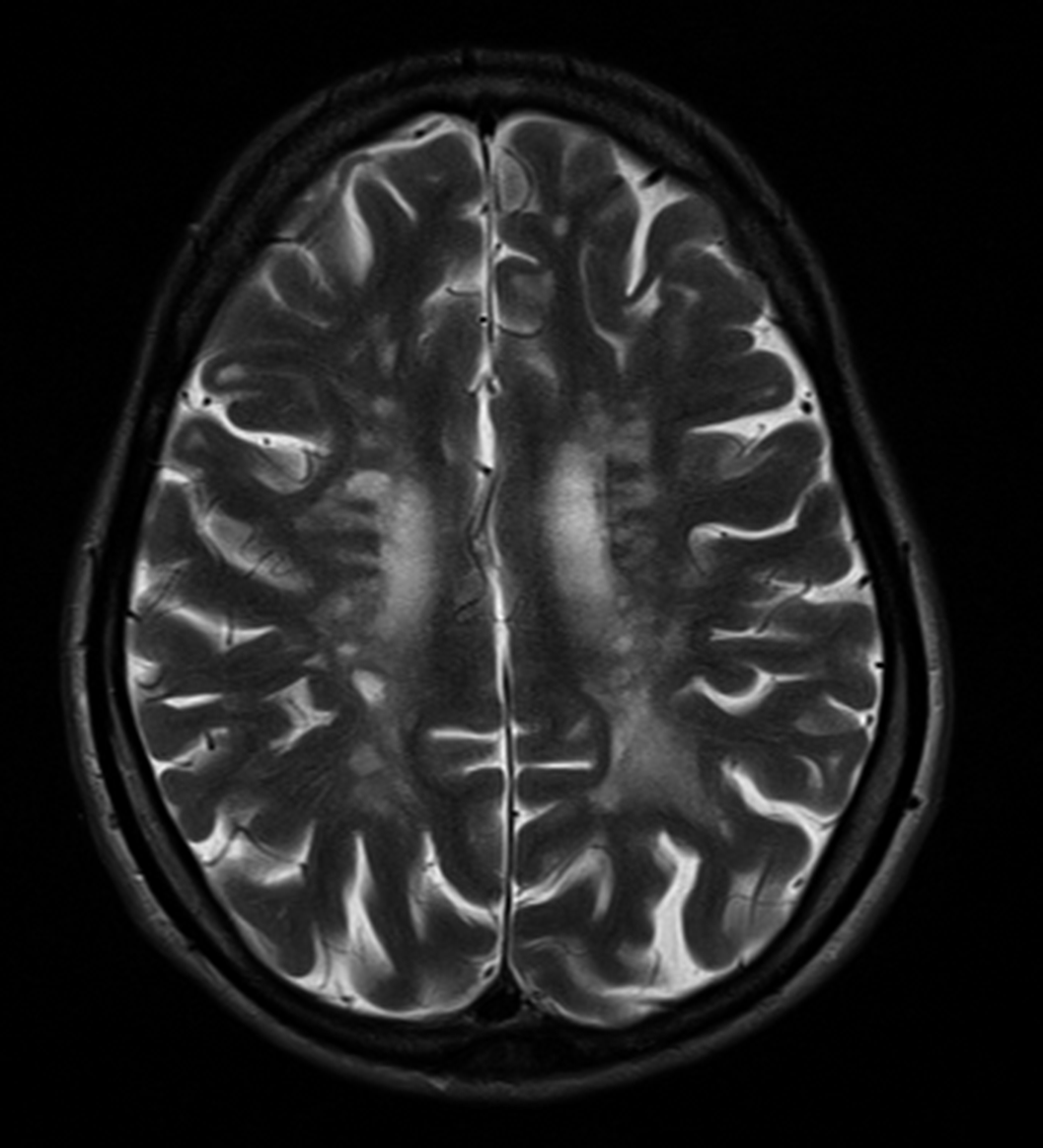
Image 2:
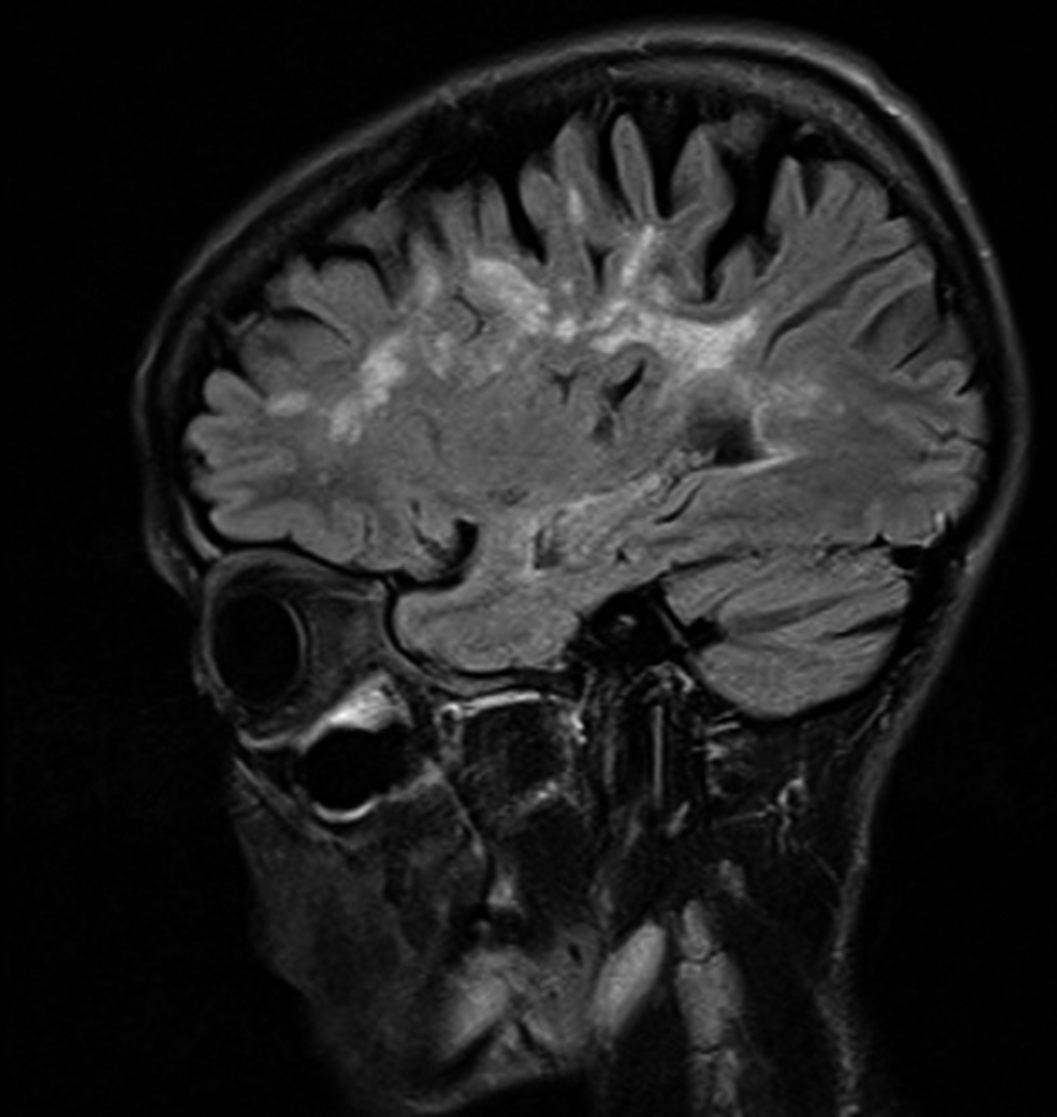 Conclusions
ConclusionsThe reformulation of the concept of cyclothymia would allow us to recognize in our patient a basic temperament of long evolution that would be the substrate on which different factors have subsequently influenced, such as antidepressant drugs or multiple sclerosis. In addition, it is necessary to know the association between BD and MS, in order to be able to offer an adequate treatment, contemplating some pharmacological options such as Lithium or some Atypical Antipsychotics, given the beneficial effect both for the affective disorder and for the neurological process.
Disclosure of InterestNone Declared
Reviewing the consistency of Dissociative Identity Disorder: a case report.
- E. Herrero Pellón, P. Albarracín Marcos, M. Huete Naval, R. Galerón Guzmán, F. Mayor Sanabria, A. Montes Montero
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S969
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 22-year-old patient who has been followed up in a daytime hospital for personality disorders since June 2022. Of note is the presence of multiple personalities (in total of more than 20 have been identified), each of which has distinct physical and psychological characteristics.
ObjectivesThe objective is to present a clinical case of dissociative identity disorder and to review the existence of scientific evidence supporting this diagnosis.
MethodsLiterature review of scientific papers over the last years and classic textbooks on the issue. We included references in English and Spanish languages.
ResultsNumerous studies support that dissociative disorders are the result of psychological traumas that generally begin in childhood. This is a difficult category to diagnose, since they present symptoms that also appear in other disorders such as those of the schizophrenic spectrum.
One or more dissociative parts of the subject’s personality avoid the traumatic memories while others become fixed to these traumatic experiences and manifest symptoms. In the case of our patient, there are dissociative episodes with subsequent amnesia and auditory, visual and olfactory hallucinations, as well as impulsive behaviors in the form of self-injury and a flattened affect, with significant emotional distancing.
Conclusions- The prevalence of dissociative identity disorder is higher than traditionally thought.
- Some theories develop how trauma essentially produces a degree of dissociation of the psychobiological systems that constitute the subject’s personality.
Disclosure of InterestNone Declared
Wernicke Encephalopathy: A case report
- M. Jiménez Cabañas, F. Ruiz Guerrero, A. Bermejo Pastor, F. Mayor Sanabria, M. Fernández Fariña, M.D. Saiz González
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S453
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We report a case of a 56-year old woman with a history of depressive disorder between 2012 and 2017 achieving full remission after treatment with antidepressants and anxiolytics. In the year 2021 was presented to the emergency department manifesting alteration of behavioral patterns, ataxia, mental confusion and horizontal nystagmus. A chronic alcohol abuse was also discovered while interviewing. She also exhibited low mood, anterograde amnesia and confabulations that improved rapidly after following treatment with thiamine.
ObjectivesReviewing clinical manifestations and treatment of Wernicke encephalopathy and the development of Korsakoff syndrome.
MethodsWe systematically reviewed articles using PubMed.
ResultsWernicke encephalopathy is a well-known complication of thiamine deficiency, mostly associated with alcohol use disorder. Classically, the syndrome comprises changes in mental status, gait ataxia and ophthalmoplegia. However, the full triad has been described in only 10-17 % of cases, which in our the case is report. After the diagnosis was established and was treated with thiamine, a rapid improvement in the patient´s clinical status was observed. Cognitive impairment was later identified, taking into account the possibility of a Korsakoff syndrome characterized by irreversible brain damage and subsequent loss of anterograde memory. In our patient, this specific diagnosis was dismissed due to the clinical improvement after thiamine treatment.
ConclusionsIt is relevant to emphasize the importance of a precise diagnosis and treatment of patients with Wernicke Encephalopathy to avoid the development of a Korsakoff syndrome.
DisclosureNo significant relationships.
Obsessive-Compulsive Disorder in children. A case report
- R. Galerón, M. Huete Naval, E. Exposito Duran, F. Mayor Sanabria, C. Regueiro Martín-Albo, F. García-Escribano Martín
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S438
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present a 9-year-old girl with celiac disease who attends a Health Center referred by her pediatrician for rituals. Her mother describes rituals from early childhood that have been intensified by the death of her grandmother from pancreatic cancer. Since then, thoughts of gluten contamination and behaviors aimed at avoiding such contamination have increased. For example, not using the common household towel and not eating until all the guests have washed their hands. If the patient does not carry out these actions, she presents significant discomfort, crying and screaming until it is done. In addition, such behaviors take up a significant amount of time.
ObjectivesTo review the literature of Obsessive-Compulsive Disorder (OCD) in children.
MethodsLiterature review of scientific articles searching in Pubmed. We considered articles in English and Spanish.
ResultsCognitive Behavioral Therapy and Sertraline up to 50mg were started. After several weeks the frequency of behaviors aimed at avoiding gluten contamination begins to decrease; as well as the anguish if these are not carried out.
ConclusionsOCD in childhood can present characteristics that differentiate it from OCD in adulthood, such as difficulty detecting obsessions and that children do not usually consider thoughts as unreal or excessive. Therefore, it is a real challenge, having to carry out an adequate differential diagnosis with other entities such as specific phobias, for adequate subsequent management.
DisclosureNo significant relationships.
Psychiatric comorbidity in epilepsy and difficulties in treatment: A case report
- M. Fernández Fariña, F. Mayor Sanabria, C. Regueiro Martín-Albo, M.E. Expósito Durán, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S462
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 36-year-old male with depressive states, impulsive traits and fits of anger (including episodes of self and heteroagressiveness) since early childhood, in the context of traumatic family history and the beginning of an epileptic disease. These symptoms have been maintained over the years, in addition to other variable and recurrent symptoms, such as severe anxiety, somatizations or serious depressive symptoms.
ObjectivesTo highlight the possible influence of epilepsy in the course of mental illnesses, especially depression, as well as the increased difficulty in management.
MethodsWe collected the complete medical history of a patient with an important history of mental health in addition to epileptic disease since childhood and we carried out a review of the comorbidity between these diseases and their treatment.
ResultsThe epileptic disease of our patient may have influenced the behavioural alterations and the depressive symptoms since childhood, as well as the personality traits with aggressiveness and impulsiveness. There is an added difficulty in treating this case given the possible interactions between antiepileptic and antidepressant medications.
ConclusionsThis case highlights the importance of taking into account the influence of this comorbidity on the prognosis of patients. Knowing the interactions and side effects of drugs is essential for good clinical management.
DisclosureNo significant relationships.
Malignant catatonia due to clozapine withdrawal: A case report and a brief review of the literature
- C. Regueiro Martín-Albo, F. Mayor Sanabria, M. Fernández Fariña, M.E. Expósito Durán, A. García Recio
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S710-S711
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Withdrawal symptoms are common upon discontinuation of many psychotropic drugs. Catatonia, a neuropsychiatric condition characterized by a number of motor, behavioral, emotional, and autonomic abnormalities, has been described as a withdrawal syndrome in a growing number of case reports, but it is not well recognized. Treatment of catatonia usually includes benzodiazepines and electroconvulsive therapy. Standard consensus states that the use of neuroleptics should be avoided, as they are thought to worsen catatonia.
ObjectivesWith this case report, we attempt to contribute to the finding in literature that the withdrawal of clozapine may be associated with catatonia, and how reintroduction of clozapine could be indicated for its treatment.
MethodsA clinical case is presented of a 37-year-old female with a history of schizophrenia, presenting with altered mental status and new onset of catatonic signs and symptoms in the setting of a 7-day emetic syndrome. The possibility that vomiting prevented proper absorption of clozapine is postulated, causing the patient to present clinical features compatible with malignant catatonia.
ResultsThe patient required treatment with benzodiazepines, electroconvulsive therapy and clozapine re-initiation, leading to improvement of catatonic symptoms within a few days.
ConclusionsThis case serves as a reminder to consider alternative diagnostic hypotheses in cases of catatonic syndrome unresponsive to standard treatments. When the clinical suspicion of drug withdrawal is high, restarting the discontinued medication, even an antipsychotic agent, may be indicated.
DisclosureNo significant relationships.
Behavioural disturbances as the clinical presentation of Wernicke Encephalopathy: a case report
- F. Mayor Sanabria, A. Bermejo Pastor, M. Fernández Fariña, M.E. Expósito Durán, C. Regueiro Martín-Albo, M. Jiménez Cabañas, C. Ortiz Sánchez-Expósito
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S473
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Wernicke Encephalopathy (WE) is the best characterized neurological complication of thiamine deficiency. Its clinical presentation can be diverse, including hallucinatory or delusional symptoms, and not necessarily associated with the classical triad of WE. This correlates with higher rates of under diagnosis. We present the case of a 72-year-old man with a history of alcoholism who was admitted to the hospital due to behavioural disturbances and subacute delusional ideas of harm.
ObjectivesTo review the epidemiology and clinical features of WE, as well as its clinical management.
MethodsReview of the literature on WE clinical presentation and management, focusing on psychopathological symptoms, applying the information to this specific case.
ResultsClassical triad of WE is only to be found in 10-17% of patients. The most common clinical presentation is changes in mental state (82%), varying from subtle changes in memory, apathy, subtle disorientation or indifference to more severe presentations such as delirium, stupor or coma. Other frequent symptoms include oculomotor dysfunction and gait ataxia. High dose thiamine supplementation therapy has proven effective in preventing clinical progression and permanent neurological damage.
Conclusions- WE is the most prevalent complication of thiamine deficiency, being associated to alcoholism in 50% of cases. - Changes in mental state is the most frequent form of clinical presentation, not necessarily associated with the classical triad of WE. - WE is a medical emergency that requires high dose thiamine supplementation therapy to prevent permanent neurological damage.
DisclosureNo significant relationships.





